Breast Cancer
Breast cancer is the most common cancer found in women.
What is breast cancer?
Breast cancer begins when abnormal cells grow in the breast. These cells may form lumps called tumours. Some tumours are cancerous (malignant) and some are not cancerous (benign). A malignant tumour can spread to other parts of the body and can be life-threatening. A benign tumour doesn’t spread to other parts of the body and isn’t usually life-threatening.

How common is breast cancer?
Breast cancer is the most common cancer found in women. It’s the second leading cause of female cancer deaths. About 1 in 7 Alberta women will have breast cancer in their lifetime.
Improvements in screening and treatments have lowered breast cancer deaths in Alberta over the last few decades.
Why is it important to find breast cancer early?
When breast cancer is found early, it’s usually very small and hasn’t spread from where it started. Treatment for cancer that’s found early may work better than for cancer that has already spread.
What are the common types of breast cancer?
There are 2 common types of breast cancer, ductal carcinoma and lobular carcinoma. Most breast cancer starts in the milk ducts (ductal carcinoma), although some start in the mammary glands (lobular carcinoma). Cancer in other parts of the breast is less common. Cancer that is “in situ” has not spread to the surrounding breast tissue. Cancer that has grown into the surrounding breast tissue is called “invasive”.
Risk factors (things you can’t change)
Not all women have the same risk (chance) of getting breast cancer. Sex and age are the 2 biggest risk factors for breast cancer. Your personal risk of developing breast cancer varies depending on several other factors (called the multifactorial nature of cancer). You have control over some risk factors. Others, such as your family history or getting older, are out of your control. See below for risk factors you can’t change.
- Sex: Women are about 100 times more likely to develop breast cancer than men.
- Age: The older a woman gets, the greater her chance of developing breast cancer. More than 3 out of 4 women diagnosed with breast cancer in Alberta are 45 years or older. Women (and those identified in the LGBTQ2S+ section) aged 45 to 74 should consider having regular screening mammograms.
- Family history: 80% of women who develop breast cancer have no family history of the disease. However, having a mother, sister or daughter with breast cancer increases your risk.
- Genetic changes: Changes in some genes, such as the breast cancer gene 1 (BRCA1) and the breast cancer gene 2 (BRCA2) can increase a woman’s risk of breast cancer. These are rare and make up less than 10% of all breast cancers.
- Personal history: Women who have had cancer in one breast have a higher risk of developing a new breast cancer in the other breast (not related to the previous one).
- Breast density: Women with dense breasts have a higher risk of getting breast cancer. Dense breasts can make it harder to find breast cancer early on a mammogram. Learn more about breast density.
- Menstrual history: Women who started menstruating (had their first period) before age 12 and/or started menopause after age 55 have a higher risk of breast cancer.
- Radiation therapy to the chest: Women who had radiation to the chest have a higher risk of breast cancer. The younger a woman was when she had radiation treatment, the higher her risk of breast cancer later in life.
Risk assessment tools
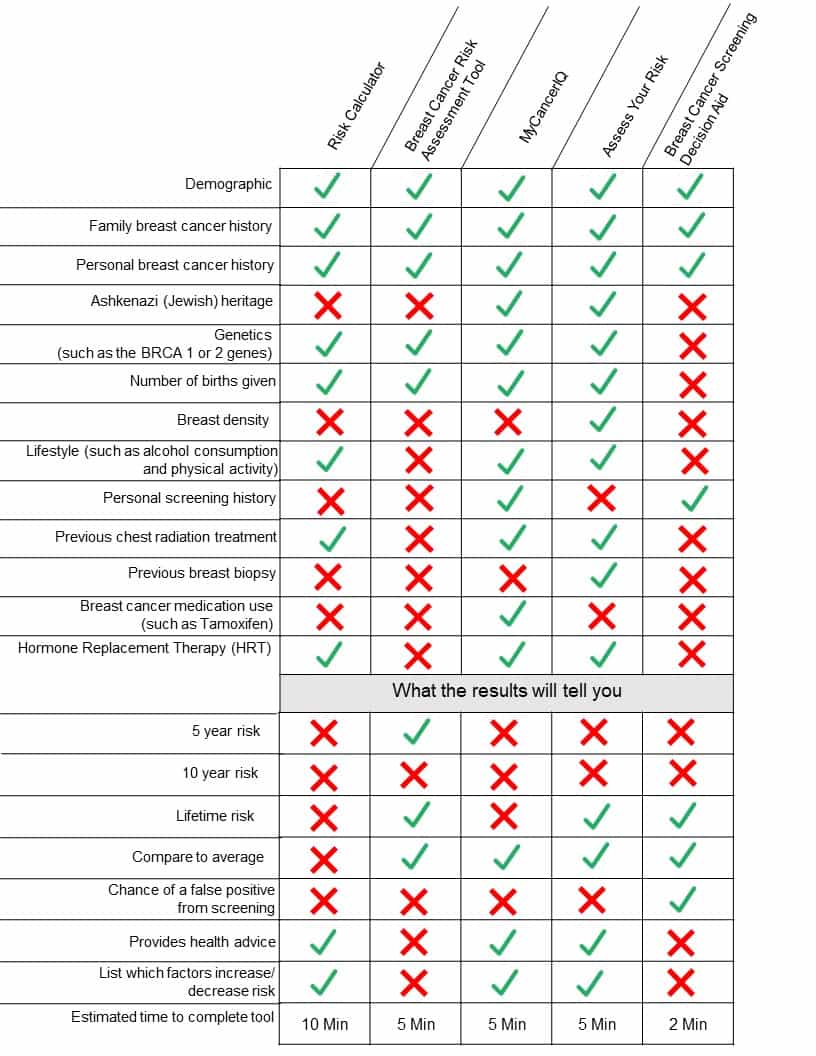
Below are links to online tools that can help you measure your risk of developing breast cancer. Each tool uses a different way of figuring out your risks, so your results might change depending on the tool you use.
- Breast Cancer Risk Assessment Tool (Gail model) by the National Cancer Institute: Tool will tell you your risk of developing breast cancer in the next 5 years or in your lifetime.
- MyCancerIQ by Cancer Care Ontario: Tool will tell you your lifetime risk of developing breast cancer in comparison to the average risk.
- Assess Your Risk by Bright Pink: Tool will tell you your risk level for breast or ovarian cancer over your lifetime. It provides helpful suggestions, such as steps you can take to lower you risk.
- Breast Cancer Decision Support Aid by the British Columbia Cancer Agency: Tool will tell you your likelihood of having breast cancer found by screening. It also provides an idea of the benefits and limitations of screening.
Breast density
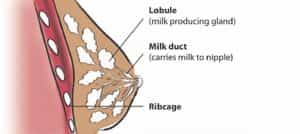 Breasts are made up of fat and other tissue such as milk ducts, lobules or glandular tissue and fibrous connective tissue. Breast density is the amount of fibrous or glandular tissue compared to the amount of fat in the breast. Dense tissue shows up as white on a mammogram, the same colour as many kinds of breast cancer. For that reason, it can be harder to find cancer when you have dense breasts.
Breasts are made up of fat and other tissue such as milk ducts, lobules or glandular tissue and fibrous connective tissue. Breast density is the amount of fibrous or glandular tissue compared to the amount of fat in the breast. Dense tissue shows up as white on a mammogram, the same colour as many kinds of breast cancer. For that reason, it can be harder to find cancer when you have dense breasts.
There are 4 categories of density, ranging from entirely fatty to extremely dense. The radiologist at the mammography clinic uses your mammogram to measure density and decide on the category. 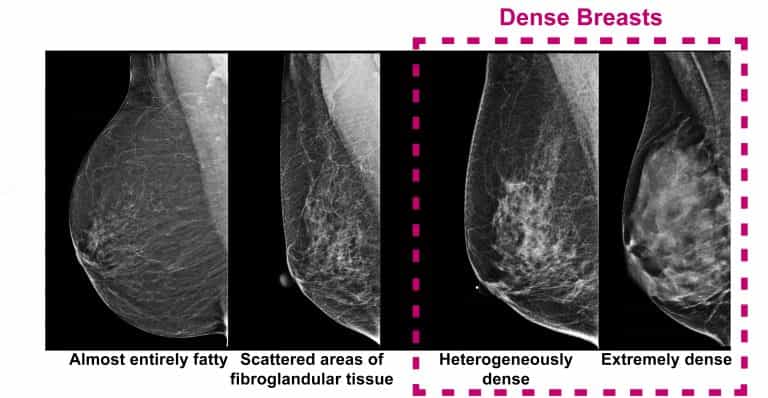
It’s very common to have dense breast tissue. Almost 50% of women aged 50 to 74 have dense breasts. There are many things that can affect your breast density including genetics, hormone levels and overall body fat. Breast density can change and also tends to go down as you age.
Dense breasts and cancer risk
Women with dense breasts have a small increase in breast cancer risk. Other factors, such as age and genetics, have a bigger impact on your overall risk of breast cancer.
How do I know if my breasts are dense?
You can’t tell how dense your breasts are by size, look or feel. The only way to find out is by having a mammogram. Some reports from your radiology clinic may mention breast density. If you aren’t sure, talk to your healthcare provider.
What should I do if I have dense breasts?
Talk to your healthcare provider about what that means for you and your personal risk. Mammography is still recommended and is the best way to find cancer early. Other tests may be offered to you in addition to your mammogram to help find breast cancer when there is dense tissue. If you’re worried about your risk of breast cancer, there are other ways to help reduce your risk such as drinking less alcohol and getting enough exercise.
If I don’t have dense breasts, should I still have screening?
If you don’t have dense breasts, you will benefit most from screening with mammography. Continue to have your regular screening mammogram as decided by you and your healthcare provider.
Reduce your risk (things you can change)
Many of the lifestyle choices you make can reduce your risk (chance) of developing breast cancer.
- Physical activity: Get regular exercise every day (ideally 30 minutes or more) — even if it’s a brisk walk or some yard work.
- Weight: Try to reach or stay at a healthy body weight. This is even more important after menopause.
- Nutrition: Try to get lots of fruits and vegetables into your diet. See Canada’s Food Guide for more information on healthy eating.
- Alcohol: Limit the amount of alcohol you drink to no more than 2 drinks per week.
- Smoking: Don’t smoke and avoid second-hand smoke. If you’re currently a smoker, talk to your healthcare provider about options for quitting or cutting back.
- Oral contraceptives: Taking the birth control pill may slightly increase your risk of getting breast cancer. The risk is small and returns to normal after you’ve stopped taking it for 10 years or more. Most women taking hormonal birth control are younger and at an age when breast cancer is rare. For women who had breast cancer in the past, hormones in the pill may have an effect on the cancer. If you’re worried about your risk of breast cancer, talk to your healthcare provider about switching to a non-hormonal form of birth control.
- Long-term hormone replacement therapies (HRT): Limit using the combination of estrogen and progestin menopausal HRT to no more than 5 years; long-term use (beyond 5 years) increases a woman’s risk of breast cancer. Within 2 years of stopping HRT, a woman’s risk of breast cancer returns to average.
- Reproductive history: Having children before the age of 30 and breast feeding both lower your risk of breast cancer.
Signs and symptoms
You don’t need to have any unusual symptoms in your breasts to need a mammogram. Having routine mammograms is the best way to find breast cancer early, before symptoms appear and when treatment may work better. Know what’s normal for you so you can notice any changes in your breasts. After all, no one knows your own body as well as you do.
See your healthcare provider right away if you notice:
- A lump in your breast or armpit
- A nipple that is pointed inward (inverted nipple), if it isn’t usually
- Crusting, bleeding or a rash on your nipple
- Unusual fluid coming from your nipple (nipple discharge)
- Dimpling or thickening of the skin in one area of your breast

Frequently asked questions
Answers to frequently asked questions about breast cancer screening not covered in the other sections can be found below.
Can women with small breasts get breast cancer?
Women with breasts of all shapes and sizes are at risk of developing breast cancer.
Do men get breast cancer?
Although men can develop breast cancer, less than 1% of all breast cancer cases in Canada occur in men. Men, like women, are encouraged to be breast aware and talk to their healthcare provider about any unusual breast changes. Based on data from the Alberta Cancer Registry, there were 24 new cases of breast cancer diagnosed in Alberta men in 2019 compared to 3,691 cases in Alberta women.
Can having a mammogram cause breast cancer or cause an already existing cancer to spread?
Mammograms need very small doses of radiation. Research confirms that the risk of harm from mammography radiation exposure is very low. The benefits of earlier breast cancer diagnosis and treatment far outweigh the risk of the small dose of radiation received during a mammogram.
Is a monthly self-exam the best way to find breast cancer early?
It’s important for women to know how their breasts normally look and feel – from the whole area of breast tissue up to the collarbone and including the armpit. While you don’t need to have a strict method for checking your breasts, talk to your healthcare provider right away if you notice any unusual changes. Learn more about when to get screened.
Do mammograms catch EVERY breast cancer?
Mammograms can miss up to 10% of breast cancer. That’s why it’s so important to go for screening mammograms regularly and to let your healthcare provider know if you notice any unusual changes in your breasts. Having dense breasts can also make it harder to find cancer on a mammogram. Learn more about breast density.
Do antiperspirants and deodorants cause breast cancer?
Several studies have been done about the link between antiperspirants and deodorants and breast cancer. So far there is no reliable evidence that they increase the risk of breast cancer. Avoid wearing deodorant containing aluminum when you go for a screening mammogram. The aluminum can show up on the mammogram images and can make breast cancers and other abnormalities harder to find.
Does cell phone use cause breast cancer?
Currently, there’s no definite link between cell phone use and increased risk of breast cancer. The International Agency for Research on Cancer concluded in 2011 that radio frequency fields, such as those from cell phones, may cause cancer but more research is needed before this can be confirmed. If you’re concerned about cell phone use and the possible link to cancer:
- Reduce the amount of time you use a cell phone or consider texting instead of talking.
- Use a headset instead of holding the phone next to your ear.
- Don’t carry your cell phone next to your skin (for example, in your bra).
Does wearing an underwire bra cause cancer?
No research shows that wearing an underwire bra increases your risk of breast cancer.
Is thermography a good breast cancer screening tool?
There is no evidence that breast thermography is an effective screening tool for finding breast cancer early. Breast thermography finds differences in skin temperature on the breast with the use of a special heat-sensing (infrared) camera. It is based on the idea that tumours can be detected by the warmth caused by increased blood flow.
Breast thermography isn’t approved by the United States Federal Drug Administration (USFDA) or Health Canada for use in breast cancer screening. In Canada, thermography equipment isn’t licensed for sale for breast cancer screening because of the lack of evidence about its effectiveness. Thermography is not covered by the Alberta Health Care Insurance Plan. Learn more from Health Canada about recall and safety alerts.
Currently, screening mammograms are the best way to find breast cancer early when treatment can work better.
Are tomosynthesis and digital mammography the same thing?
Digital mammography (sometimes shortened to 2D mammo) takes 2 x-ray images of each breast during a screening exam. Tomosynthesis (sometimes shortened to Tomo, DBT, or 3D mammo) takes x-rays of the breast, like a digital mammogram. However, this newer technology takes multiple pictures from different angles, making a 3D-like videos of the breasts.
Can tomosynthesis be used instead of mammography for breast cancer screening?
Tomosynthesis isn’t recommended for breast cancer screening on its own. It’s sometimes added (supplemental) to digital mammography during screening. As tomosynthesis takes more pictures, it may provide some additional benefits to mammography done without tomosynthesis. People at higher risk of breast cancer may benefit more when tomosynthesis is added. However, this should be based on overall risk and not just on one factor, such as breast density. Talk to your healthcare provider about your personal risk for breast cancer.
There are several risk assessment tools listed above that you can use to assess your risk for breast cancer. Keep in mind that supplemental tomosynthesis is still being studied to see if it’s an effective screening tool for population-based screening programs. It isn’t clear yet if people have better outcomes (for example, if they live longer when breast cancer is found earlier) when screened with tomosynthesis in addition to digital mammography.
Will the COVID-19 vaccine impact my mammogram result?
There have been some recent reports of an uncommon occurrence that receiving the COVID-19 vaccine just prior to having a mammogram may slightly increase your chance of getting a false positive (being called back for more testing when you do not actually have breast cancer). As a result, your provider may ask about your recent COVID-19 vaccination history when you book your mammogram. They may also suggest you book the mammogram appointment 4-6 weeks after your COVID-19 vaccination, as there is a chance you may experience some side effects, such as large lymph nodes in one or both arm pits.
If you’d like to read more information about this, you might want to check out these articles:
Should I get screened for breast cancer with the new blood test I’ve been hearing about?
You may have heard about a new blood test by Syantra DX to help screen for breast cancer. At this time, the test is not recommended as part of breast cancer screening. If you’re interested in this test, here are a few things to be aware of:
1) It is experimental. The test is still in clinical trials and data on how well it works is only inferred based on early results.
2) If you’re between the ages of 45 and 74, you still need to get a screening mammogram. The blood test is not meant as a substitute for screening mammography. Any statistics about its effectiveness are based on having both a screening mammogram and the blood test.
3) The test is not covered as part of your Alberta Health Care Insurance Plan.
Remember, screening mammograms are still the best way to screen for breast cancer and they are covered as part of your Alberta Health Care Insurance Plan.
Why did you change the guideline to start screening at 45 years old instead of starting at 50 years?
The recommendation was made based on new evidence in the literature, epidemiology of breast cancer in Alberta and simulation modeling outcomes using Alberta data. It was determined that the benefits of breast cancer screening outweigh the potential harms for women aged 45-49.
Eligible women, transgender, gender diverse, and non-binary people have always had the choice to start breast cancer screening from age 40 years in Alberta. Click here to learn about the benefits and risks of mammograms.







