Get Screened
Having regular colorectal cancer screening can prevent and detect cancer at its early stages when treatment is more effective.
Why get screened?
Colorectal cancer is one of the most common cancers in Alberta and affects about 1 in 19 men and 1 in 21 women in their lifetime. Although colorectal cancer can happen at any age, your risk of getting it increases as you get older. Learn more about risk factors that may increase your risk. If you’re between the ages of 50 and 74, it’s important to get screened regularly.1
What is colorectal cancer screening?
Colorectal cancer screening (or colon cancer screening) means looking for early signs of cancer in people who feel well and have no symptoms. Colorectal cancer is easier to treat when found at an early stage. In fact, 90% of cases can be treated successfully if they’re found early.
Although colorectal cancer can happen at any age, your risk of getting colorectal cancer increases as you age. About 90% of cases are in people 50 years of age or older. In Alberta, it’s recommended that individuals aged 50 to 74 years get screened with the fecal immunochemical test (FIT) every year. After age 74 the benefits of screening may no longer outweigh the risks. Speak with your healthcare provider about your risk for colorectal cancer and when screening may no longer be of benefit.’
Next to age, family history is the most common risk factor for colorectal cancer. If you have a family history of colorectal cancer or polyps, it’s a good idea to talk to your healthcare provider about when you should get screened. Certain risk factors such as family history means you may need to start screening at age 40 or even younger.
The 2 main screening tests for colorectal cancer are:
- Fecal immunochemical test (FIT) test This test looks for blood in your stool (poop) that you can’t see. It’s an easy test that you can do at home. If blood is found in your poop, you will need a colonoscopy to make sure the blood isn’t caused by cancer.
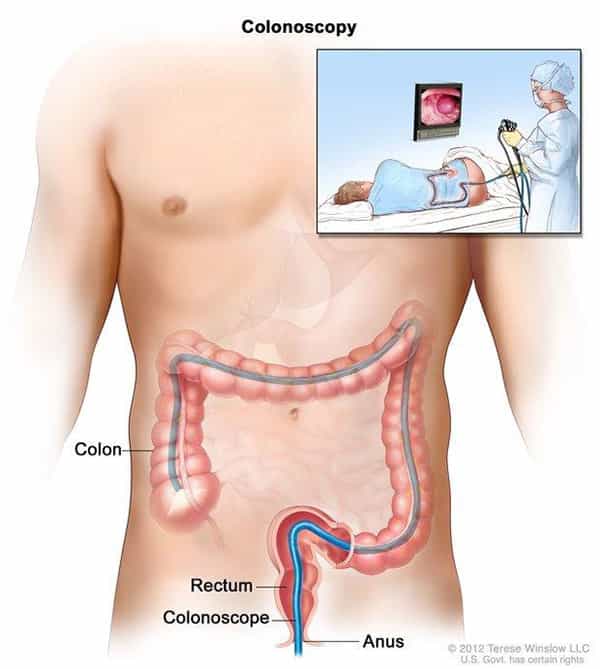
- Colonoscopy: This test lets a healthcare provider see the inside lining of your rectum and colon. This is done with a long, flexible tube called a colonoscope. If polyps or tissue growths are found they can be removed during the test.
Both tests find problems early and help save lives. Talk to your healthcare provider about which screening test is right for you and how often you need to have it. Learn more about which test may be right for you.
1. Toward Optimized Practice. Colorectal Cancer Screening Clinical Practice Guideline. November 2013. 2. 2019 Report on Cancer Statistics in Alberta. Surveillance & Reporting. Cancer Research & Analytics, Alberta Health Services.
Who should get screened?
If you’re 50 to 74 years of age, you should get screened regularly. Think of it as part of your regular health routine. If you have a family history of colorectal cancer you may need to start screening at age 40 or younger.
Find out which test may be right for you:
| If… | Then… |
| You’re 50 to 74 years old and have no personal or family history of polyps or colorectal cancer … | Screen with the FIT home stool test every year. |
| You have a first degree relative (parent, sibling or child) that’s had colorectal cancer and/or high risk adenomas, especially if they were younger than 60 when they got it…
Or… You’ve had colorectal cancer before or have been told you have polyps in your colon… |
Colonoscopy is the recommended screening test.
Ask your healthcare provider when you should be screened. Risk factors such as personal or family history may mean you should start screening at age 40 or even younger. |
If you have symptoms of colorectal cancer at any age, talk to your healthcare provider right away.
Symptoms may include:
- Rectal bleeding
- A change in your bowel habits
- Pain in your abdomen
- Losing weight and you don’t know why
Your symptoms may be caused by something other than cancer but to know for sure you can speak to your healthcare provider. Learn more about signs and symptoms at MyHealth.Alberta.ca.
What is a FIT?
The fecal immunochemical test (FIT) is used to screen for colorectal cancer in people aged 50 to 74 who have an average (or normal) risk for getting the disease. People with an average risk have no personal or family history of the disease. Anyone aged 50 to 74 who is at average risk should screen with FIT every year.
What to expect with FIT
A FIT checks your stool (poop) for traces of blood that you can’t see. It’s safe, easy to do and can be done in the privacy of your own home.
How do I get a FIT kit?
There are 2 easy ways to get a free FIT kit:
1. Talk to your healthcare provider. They’ll give you a lab requisition form. Take this form to the lab to pick up your FIT kit.
2. Order online at screeningforlife.ca or call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926. We’ll mail you a FIT kit.
If you need a healthcare provider:
• Visit albertafindaprovider.ca
• Call Health Link at 811
How do I do a FIT?
The FIT kit comes with easy to follow instructions. You’ll collect a small sample of stool (poop) from 1 bowel movement. After collecting your sample, you’ll take your completed FIT kit back to the lab. The lab will test the sample for any hidden blood.
FIT Lab Instructions [info sheet]
Getting your FIT results
Your FIT result will be sent to your healthcare provider who will follow-up with you directly. Learn more about getting your FIT results.
Benefits and risks of FIT
As with any test, there are both benefits and risks.
Benefits of doing a FIT
A FIT is easy to do, safe and won’t hurt. It can detect traces of blood in your poop that you can’t see. If any blood is found, the recommended follow-up test is a colonoscopy. A colonoscopy may find any precancerous polyps or cancer at its early stages, when treatment can work better.
Risks of doing a FIT
A FIT could miss blood in the poop, because a polyp or cancer may not bleed at the time you take the test. This is why screening with FIT every year gives you the best chance of colorectal cancer being found early, when treatment can work better.
Frequently asked questions about ordering a FIT kit
I don’t have a healthcare provider (for example, a family doctor). Can I still order a FIT kit?
Yes, you can still order a FIT kit online or by phone. If your FIT result is abnormal, it’s important that you make an appointment with a healthcare provider to discuss follow-up testing. If you need help finding a healthcare provider albertafindaprovider or call Health Link 811.
My healthcare provider gave me a requisition form to take to the lab and pick up my FIT kit. Can I order it online instead and have it mailed to me?
No, if you already have a lab requisition for a FIT kit, please take this form to your nearest lab and pick up your FIT kit instead of ordering one.
How will my FIT kit be shipped?
Your FIT should arrive by Canada Post, in a discrete envelope, within 10 business days. If it’s been over 3 weeks and your FIT kit has still not arrived, call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926, Monday to Friday, 8:00 a.m. to 4:30 p.m.
My FIT kit was lost or damaged. Can I order a new one?
Call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926, Monday to Friday, 8:00 a.m. to 4:30 p.m. to order a new FIT kit.
I am having a problem with my FIT kit order. What should I do?
For assistance, call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926, Monday to Friday, 8:00 a.m. to 4:30 p.m.
Completing your FIT:
I made a mistake collecting my stool sample. What should I do?
Call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926, Monday to Friday, 8:00am to 4:30pm to order a new FIT kit.
I got my FIT kit in the mail a while ago but haven’t done it yet. Does the test expire?
Yes, the test does expire. Check the expiry date on your FIT collection container. If your FIT has expired, please discard. Call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926, Monday to Friday, 8:00am to 4:30pm, to order a new FIT kit.
How soon after collecting my sample do I take it to the lab?
You need to take your FIT and lab requisition form to the lab within 7 days of collecting your sample.
Do I need to make a lab appointment to drop off my completed FIT?
No, you do not need an appointment to drop off your FIT kit.
Where is my nearest lab for FIT drop off?
For lab locations and hours of operations visit:
- Albertaprecisionlabs.ca or call 1-877-868-6848
How do I get my results if I ordered my FIT kit?
You can view your FIT results online if you have a MyChart (formerly MyAHS Connect) account. MyChart is available to all MyHealth Records users. Sign up for MyChart by creating a verified Alberta.ca account and registering for MyHealth Records.
If you have an abnormal FIT result you will receive a result letter in the mail. A nurse from Primary Care Alberta will call you to discuss the next steps.
Normal result letters will not be mailed to Albertans who have a MyChart account.
Will my results be sent to my healthcare provider if I ordered my FIT kit online or by phone?
If your result is abnormal you will need to make an appointment with your healthcare provider to discuss the need for a colonoscopy. If you do not have a healthcare provider a nurse from Primary Care Alberta will provide you with some resources to help you find a healthcare provider in your area.
You will need to book an appointment with your healthcare provider as soon as possible to discuss your abnormal result and follow-up testing.
What is a colonoscopy?
A colonoscopy lets your doctor see the inside lining of the colon and rectum. This is done with a colonoscope, which is a long, thin, flexible tube with a light and small video camera on the end. This test will help your healthcare provider know if there are polyps or cancer in the colon and or rectum.
To get a colonoscopy in Alberta you need a referral from your healthcare provider or a provider at a walk-in clinic. If a colonoscopy is the right test for you, your healthcare provider will recommend you having this test and arrange your referral. A colonoscopy is not a test you can request or arrange on your own.
Why is a colonoscopy is done?
Your healthcare provider may recommend a colonoscopy to:
· Follow up after an abnormal fecal immunochemical test (FIT) result. An abnormal FIT result means blood was found in the stool (poop). When blood is found, it’s important to find out what may have caused it. Most often, a colonoscopy is recommended.
· Check on symptoms. A colonoscopy can help your healthcare provider investigate and find the cause of symptoms such as rectal bleeding, abdominal (belly) pain, a change in bowel habits, and unexplained weight loss.
· Monitor after colorectal treatments. (for example, a colonoscopy, surgery or cancer treatment).
· Screen for colorectal cancer. If you have a personal or family history of colorectal cancer or high-risk polyps (a type of polyp that can turn into cancer if it’s not removed) your healthcare provider may recommend a screening colonoscopy test.
Watch these 2 short videos to learn more about colonoscopy.
Video 1: What is a colonoscopy and why do I need one? (05:38)
Learn about the colonoscopy, and its benefits, and risks.
Printable handout:
My doctor wants me to have a colonoscopy
Video 2: What to expect during and after your colonoscopy (07:41)
This video will guide you through the colonoscopy process.
The risks and benefits of getting a colonoscopy
Benefits of a colonoscopy
There are many benefits of having a colonoscopy.
It can help diagnose problems in the bowel and can also prevent colorectal cancer by finding and removing polyps. When colorectal cancer is found early, 90% of cases can be treated successfully.
The number of people who benefit from a colonoscopy is much higher than the number who have problems. Talk to your healthcare provider if you have any questions or want to discuss alternatives to a colonoscopy.
Risks of a colonoscopy
Overall, a colonoscopy is safe. But, like any medical test, there’s a small chance that problems can occur.
· Before having a colonoscopy, you’ll need to drink a strong laxative medicine to clean out your colon. This can sometimes cause nausea, vomiting, dehydration, or dizziness. Severe dehydration can cause falls, electrolyte imbalances, or kidney issues. Electrolytes are minerals that your body needs. The best way to prevent dehydration is to drink lots of clear fluids.
· For the test, most people have sedation medicine through an intravenous line or IV to help them feel calm and comfortable. In rare cases, sedation medicine can cause problems such as low blood pressure, breathing difficulties, or allergic reactions.
· Although the test is thorough, there’s a chance that cancer or polyps could be missed.
· Bleeding can happen where a polyp is removed, or a tissue sample is taken.
· Rarely, a colonoscopy can cause a hole or tear in the colon.
· Infection can occur in the colon, or at the IV site.
· If a serious problem happens, you might need surgery, antibiotics, or a blood transfusion. In extremely rare cases, damage to nearby organs or a serious complication from a colonoscopy can result in death.
More information
To find out more about colonoscopy, go to ahs.ca/colonoscopy or speak with your healthcare provider.
Where to get screened
In Alberta, getting screened can be done easily at home. If you’re 50 to 74 years old there are 2 easy ways to get a free FIT kit.
- Talk to your healthcare provider about colorectal cancer screening. If FIT is the right test for you, they’ll give you a lab requisition form. Take this form to the lab to pick up your FIT kit.
OR
- Order online at screeningforlife.ca or call Primary Care Alberta Screening Programs toll free at 1-866-727-3926. We’ll mail you a FIT kit.

If you don’t have a healthcare provider, check out these resources to help find one:
- Visit Albertafindaprovider.ca
- Call Health Link at 811
Remember, getting screened is the most important thing you can do to protect yourself against colorectal cancer.
Other colorectal cancer screening tests
While the FIT and colonoscopy are the 2 most common screening tests, other screening tests are also available. Any abnormal results should still be followed by a colonoscopy for the tests described below. Talk with your healthcare provider about which screening test is right for you.
- CT colonography: This is a computed tomography (CT) scan taken of the colon after bowel cleansing to get an accurate picture of the lining of the rectum and colon. This test is usually done at private radiology clinics and is not covered by the Alberta Health Care Insurance Plan. If a polyp is found, it’s recommended that you have a colonoscopy to remove the polyp, as the CT only looks at your colon.
- Flexible sigmoidoscopy: This test uses a colonoscope to examine only the lower left side of the large bowel. If a polyp is found, it’s recommended that you have a colonoscopy to examine the other side of the colon. A flexible sigmoidoscopy is usually done every 5 years.
Research into new colorectal cancer screening tests.
- Shield™: A new blood test for colorectal cancer screening. Shield™ detects DNA molecules shed by cancer and pre-cancer cells into the bloodstream. If cancer cells are detected the patient will need to have a follow-up colonoscopy. Shield was recently approved by the FDA for use in the Unites States. Currently it’s not a recommended colorectal cancer screening test in Alberta or anywhere in Canada. The Alberta Colorectal Cancer Screening Program will continue to review the evidence for the use of this test as it becomes available.
- PolypDX™: Alberta is starting to test a new approach to colorectal cancer screening using a urine test called PolypDX™. This test detects pre-cancerous polyps in the colon. If polyps are found, the follow-up test is a colonoscopy. PolypDX™ isn’t available to Albertans.
Colorectal Cancer Screening for the 2SLGBTQI+ Community
We’re keeping up with the latest research about cancer screening for 2SLGBTQI+people. We’ll be regularly updating this section with input from our 2SLGBTQI+ partners and emerging evidence.
Last updated December 2023.
Screening Programs is pleased to share three new information sheets on cancer screening that have been designed for the 2SLGBTQI+ community.
Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Breast/Chest Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Cervical Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Colorectal cancer screening is for everyone
It’s important for everyone of any gender identity or sexual orientation to get screened for colorectal cancer between the ages of 50 to 74. Sexual orientation or gender identity doesn’t affect your risk of colorectal cancer and won’t change how you’re screened.
Get screened every year using the fecal immunochemical test (FIT). FIT is an easy at-home screening test that checks for hidden blood in your stool (poop).
Receptive anal sex (bottoming) and colorectal cancer screening
You can keep having anal sex before and after you’ve had a FIT or colonoscopy.
Gender-affirming hormone therapy and colorectal cancer
We don’t know if testosterone, estrogen or progesterone are risk factors for colorectal cancer. There’s no evidence either way. What we do know is that healthcare providers don’t need to know a person’s hormone levels when screening for colorectal cancer. For example, a healthcare provider won’t ask someone if they’re on birth control.
Citations: Canadian Cancer Society
How Can I Get Screened?
There are 2 easy ways to get a free FIT kit:
1. Talk to your healthcare provider. They’ll give you a lab requisition form. Take this form to the lab to pick up your FIT.
2. Order online at screeningforlife.ca or call Primary Care Alberta Screening Programs toll-free at 1-866-727-3926. We’ll mail you a FIT.
If you need a healthcare provider:
• Visit albertafindaprovider.ca
• Call Health Link at 811
Gender affirming clinics and providers:
- DX Medical Centres – Medical Clinic in Edmonton
- Wellness Centre in Edmonton
- Dr. Jillian DeMontigny (Haig West Family Health Care Clinic in Lethbridge)
- Justik Medical Clinic – Family Medicine Clinic in Edmonton
- Dr. Ted Jablonski and others (Pinnacle Medical Centres in Calgary and surrounding area)
- Skipping Stone
- Telus Virtual Health (province-wide)
- The Alex in Calgary
- The Pride Centre in Edmonton
- Trans Wellness Initiative (province-wide)
Gender affirming clinics and providers – Indigenous:
- Elbow River Healing Lodge in Calgary
- Indigenous Wellness Clinic in Edmonton
- Dr James Makokis (South Common Medical Clinic in Edmonton)
*Please note, some clinics may not be accepting patients at this time. Contact the clinic directly to find out if they are accepting patients, have a waiting list, or can provide a referral.
For More Information
Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Breast/Chest Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Cervical Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
LGBTQ2S+/Sexual and Gender Diversity, Alberta Health Services
Sexual and Reproductive Health, Alberta Health Services
For 24/7 nurse advice or general health information, call Health Link at 811.
Colorectal Cancer Screening for First Nations People
The following resource about colorectal cancer screening was developed for First Nations people by the Alberta First Nations Information Governance Centre. Alberta FNIGC Colorectal Screening




