Get Screened
Why get screened?
Screening mammograms are the best way to find breast cancer early, when treatment may work better.
Who should get screened?
If you’re 45 to 74 years of age, start making mammograms part of your regular health routine. The risk (chance) of breast cancer increases as you get older. Follow these guidelines to know when to get screened:
- Women younger than 40: The risk of breast cancer at this age is low. Generally, screening mammograms aren’t needed before the age of 40. Talk to your healthcare provider if you’re concerned about having an increased risk of breast cancer.
- Women 40 to 44: It’s less clear that the benefits of mammograms outweigh the risks for women in this age group. Talk to your healthcare provider about your breast cancer risk and your need for mammograms.
- Women 45 to 74: Breast cancer screening is proven to have the most benefit within this age range. Have a mammogram every 2 years or as decided by you and your healthcare provider.
- Women 75 and older: The benefits of continuing to screen once you turn 75 depend on your personal health (how healthy you are overall). Talk to your healthcare provider about whether or not continuing to screen is right for you. If you choose to continue screening, the Alberta Breast Cancer Screening Program in Primary Care Alberta will no longer send you reminder letters to screen once you turn 75.
Unsure if breast cancer screening is right for you? Try a Risk Calculator.
What if I have breast implants?
Breast cancer screening is still very important if you have breast implants. Implants can interfere with screening mammograms, so you’ll need more images in order to detect (find) abnormal changes. Remember to let the radiology clinic know that you have breast implants when booking your mammogram appointment.
What is a mammogram?
A mammogram is an x-ray of the breast. There are 2 different kinds of mammograms: screening and diagnostic.
Screening mammograms
Screening mammograms are regular checks used to find early signs of cancer in women who have no noticeable breast problems or symptoms. They can find abnormal changes in the breast that are too small to be felt by you or your healthcare provider. If your screening mammogram finds any abnormal changes, your healthcare provider may recommend having a diagnostic mammogram.
Diagnostic mammograms
Diagnostic mammograms take more images for a closer look at the area of concern found on a screening mammogram. They’re also used for women who’ve had breast cancer before or who notice unusual breast changes, such as:
- A new lump in the breast or armpit
- A nipple that’s pointed inward (inverted nipple), if it isn’t usually
- Crusting, bleeding or a rash on the nipple
- Unusual fluid coming from the nipple (nipple discharge)
- Dimpling or thickening of the skin in one area of the breast
If you think you need a diagnostic mammogram, speak to your healthcare provider for a referral.

If you don’t have a healthcare provider, check out these resources to help find one:
- Visit Alberta Find a Doctor
- Call Health Link at 8-1-1
- Visit Inform Alberta
- Visit College of Physicians and Surgeons of Alberta
What to expect with a mammogram
You might have a few questions about how a mammogram is done. The process itself should only take about 10 minutes and will be done by a female technologist to help you feel comfortable and at ease.
How should I prepare for a mammogram?
On the day of your appointment you should:
- Wear a separate top and bottom as you’ll have to remove clothing from the waist up.
- Avoid wearing perfume, antiperspirant, deodorant and body powder. These can affect the mammogram results.
What happens during a mammogram?
Once you’re standing in front of the mammography machine:
- One breast at a time is positioned (placed) on the machine. The machine will be adjusted to your height.
- A second plate will press down on your breast for a few seconds to spread out the breast tissue so that small abnormalities can be seen.
- For a screening mammogram, 2 x-rays will be taken of each breast; 1 from the top and 1 from the side. Several more x-rays are taken for diagnostic mammograms. If tomosynthesis is used, multiple x-ray images are taken to create a video-like view of each breast. Learn more about tomosynthesis under frequently asked questions.
- These x-rays will then be looked at by a radiologist for any abnormal changes.
- Once the exam has been reviewed by a radiologist, you’ll receive a result letter in the mail from the Alberta Breast Cancer Screening Program. Learn more about getting your mammogram results.
Does a mammogram hurt?
Your breasts need to be compressed (flattened) to get the best image possible. This may be uncomfortable or slightly painful, but tolerable. Each compression only lasts a few seconds, so any discomfort will be very short. If you normally have tender breasts, you may find it more comfortable to have your mammogram at least a week before or after your period.
Find out why compression is important when having a mammogram from the BC Cancer Agency Screening Mammography Program.
Benefits and risks of a mammogram
Mammograms are generally very safe. However, as with any procedure, having a mammogram has both benefits and risks.
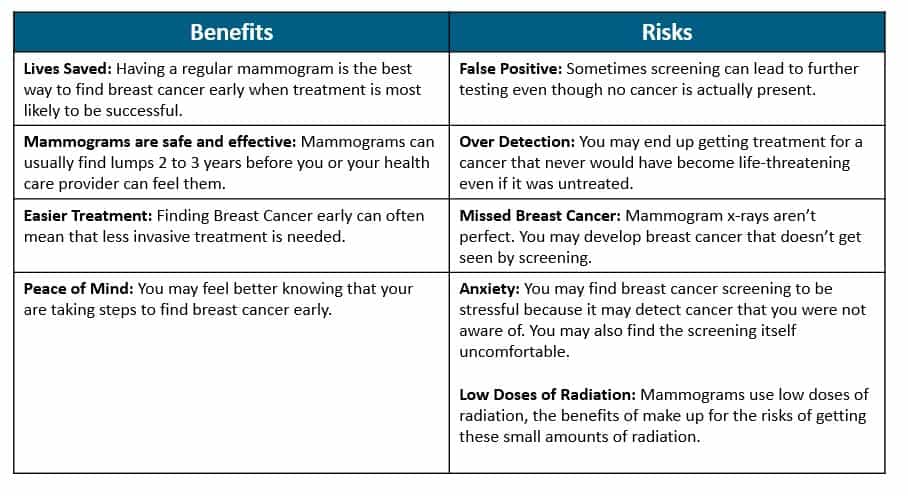
Informed decision making: Screening for breast cancer is a choice. Make your choice by carefully thinking about the benefits and risks of breast cancer screening. You may experience these benefits or risks in a different way than others. You’ll have to decide for yourself if you think the benefits are worth more than the risks. Talk about this with your healthcare provider to help you decide if screening is right for you.
Review the resource below to help you think about how the benefits and risks of breast cancer screening fit with your own personal values.
Making an informed decision about breast cancer screening [booklet]
Nurse Navigator pilot project for breast cancer screening
Breast cancer screening for Albertans without a primary care provider
Pilot project led by the Alberta Breast Cancer Screening Program in partnership with the Alberta Society of Radiologists.
What is the Nurse Navigator pilot project?
The Nurse Navigator project is a new pilot project that ensures eligible Albertans without a primary care provider can access breast cancer screening (screening mammograms) and any necessary follow-up testing under the supervision of a physician.
Who is eligible?
The pilot project is available province wide at participating radiology clinics for average-risk women, and eligible 2SLGBTQI+ individuals, aged 45 to 74 who do not have a primary care provider and have an Alberta Health Care card.
Anyone aged 40 to 44 who has been previously screened or referred for screening is also eligible. This ensures that individuals in this age group have had a conversation with a healthcare provider about the benefits and risks of screening before the recommended starting age.
How does it work?
The clinic where you were screened will ask if you would like to use the Alberta Breast Cancer Screening Program as your referring provider for your mammogram. Once you provide consent, your screening results will be sent to the Nurse Navigator who will review them. A result letter will also be sent to you directly by the radiology clinic. Your results can also be viewed electronically on MyChart (formerly MyAHS Connect)/MyHealth Records. If necessary, the Nurse Navigator will contact you to discuss the results.
What are the benefits of using the Nurse Navigator?
If your mammogram results are abnormal, a Nurse Navigator will help you understand the results and assist in arranging any necessary follow-up testing under the guidance of a physician. They can also provide resources to help you find a primary care provider so that you can receive more personalized care.
If your results are normal, you will not receive a phone call.
Do I have to participate?
No, you don’t have to participate in the pilot project. However, please be aware that your radiology clinic may require a referring provider to ensure follow-up in the event of abnormal results.
Remember: Regular mammograms are the best way to detect breast cancer early, before symptoms appear, when treatment is more effective.
Where to get screened
Mammograms are done at specific radiology clinics, some hospitals and through mobile screening clinics through Primary Care Alberta Screen Test that travels to over 120 rural communities throughout Alberta. The requirements for booking a screening mammogram in Alberta are different depending on your age:
- Women aged 40 to 44: You need a referral from your healthcare provider for your first screening mammogram. After your first mammogram, you can book your regular appointment by providing the name of your healthcare provider at a radiology clinic of your choice.
- Women aged 45 to 74: You can book a screening mammogram without a referral. In Alberta, some clinics may need women to have a healthcare provider to book a screening mammogram. This is so that the clinic knows who to send the results to and who will do the follow-up, if needed.
- Women aged 75 and older: If you choose to continue screening, you’ll need a referral from your healthcare provider.
If you’re ready to book your screening mammogram, visit Where to Get Screened to find a complete list of locations, including mobile clinic sites.
Breast/Chest Cancer Screening for the 2SLGBTQI+ Community
We’re keeping up with the latest research about cancer screening for 2SLGBTQI+ people. We’ll be regularly updating this section with input from our 2SLGBTQI+ partners and emerging evidence.
Last updated December 2023.
Screening Programs is pleased to share three new information sheets on cancer screening that have been designed for the 2SLGBTQI+ community.
Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Breast/Chest Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Cervical Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Words are Important
We recognize that many gender diverse people may use different words for their body parts. We use the biological terms as a practice, but patients have the right to request that their healthcare providers use different words for their safety and comfort.
Should I get screened?
If you have breast tissue, it’s important to consider your need for screening mammograms. Breast tissue is the fatty tissue on top of the chest muscles. People of any gender identity or sexual orientation may need screening mammograms.
Before getting screened, it is recommended to speak with your healthcare provider about your personal cancer risk level and whether screening is right for you.
When are screening mammograms recommended?
Consider having screening mammograms regularly if you’re between the ages of 45 to 74 and you have breast tissue. This includes if:
- You’ve taken gender affirming hormones (like estrogen) to increase the size of your breasts for 5 or more years in total. The years do not have to be back-to-back.
- You haven’t had top surgery to remove breast tissue, even if you’ve had a hysterectomy or are taking testosterone. Testosterone therapy isn’t believed to significantly increase the risk (chance) of breast/chest cancer.
Remember, it’s important to get screening mammograms regularly, even if:
- You have no family history of breast/chest cancer
- You’re a lesbian, bisexual, or queer woman
- You’ve had a hysterectomy
- You’re taking testosterone
- You’ve been through menopause
- You feel healthy and have no symptoms of breast/chest cancer
When are screening mammograms not recommended?
Screening mammograms are not recommended if you do not have breast tissue. This includes if:
- You’ve taken gender affirming hormones (like estrogen) to increase the size of your breasts for less than five years.
° It’s still important to have counselling around breast self‑awareness and regular physical examinations to check the amount of breast development. - You’ve had top surgery to remove breast tissue
° Chest self‑awareness and regular physical exams are recommended because usually some original breast tissue will remain after surgery. Talk to your healthcare provider about how to best monitor your chest health.
Frequently Asked Questions about Breast/Chest Cancer Screening for the 2SLGBTQI+ Community
I had a hysterectomy, do I need breast/chest cancer screening with mammography?
You should still have regular breast/chest cancer screening with mammography even if you’ve had a hysterectomy, unless you have had top surgery. Talk to your healthcare provider about how to best monitor your breast/chest health.
I have breast/chest implants; should I and can I still get screened for breast/chest cancer with mammography?
Breast/chest cancer screening is still important if you have breast implants. Special techniques are used to make sure the most amount of breast/chest tissue is seen in the image and to make sure that the implant doesn’t rupture. Be sure to mention that you have breast/chest implants when booking your mammography appointment as more time might be needed to ensure the best image is taken. Talk to your healthcare provider about how to best monitor your breast/chest health.
I bind my chest, does this increase my chance of getting breast/chest cancer?
The risks of breast/chest cancer from chest binding haven’t been well studied, so it’s not clear at this time if it has any impact on breast/chest cancer risk. Currently, there is no evidence to suggest that binding increases the risk of breast/chest cancer.
However, it is important to check-in with your healthcare provider to monitor your breast/chest health while binding.
**************
Screening can be worrying for some people due to previous trauma, gender dysphoria, or a lack of trust in healthcare settings. It can be difficult to make breast/chest screening a priority, especially if you’re concerned about experiencing discrimination. All patients have the right to receive healthcare without discrimination. Talk to your healthcare provider about your personal screening needs and ways to make screening more comfortable for you.
How can I get screened?
If you’re between the ages of 45 to 74, you can book a screening mammogram without a doctor’s referral. Use the “Where to Get Screened” tool to find a radiology clinic most convenient for you. If you’re between the ages of 40 to 44 or over 74 years old, we encourage you to talk with your healthcare provider about what would be best for you.
Questions to consider:
When booking an appointment, you may be asked if you have breast implants, have had top surgery, or are taking hormones. This is because these factors may affect the appearance of your screening images.
If you need a healthcare provider:
• Visit albertafindadoctor.ca
• Call Health Link at 8-1-1
• Visit search.cpsa.ca
(College of Physicians & Surgeons of Alberta)
Gender affirming clinics and providers:
- DX Medical Centres – Medical Clinic in Edmonton
- Wellness Centre in Edmonton
- Dr. Jillian DeMontigny (Haig West Family Health Care Clinic in Lethbridge)
- Justik Medical Clinic – Family Medicine Clinic in Edmonton
- Dr. Ted Jablonski and others (Pinnacle Medical Centres in Calgary and surrounding area)
- Skipping Stone
- Telus Virtual Health (province-wide)
- The Alex in Calgary
- The Pride Centre in Edmonton
- Trans Wellness Initiative (province-wide)
Gender affirming clinics and providers – Indigenous:
- Gender affirming clinics and providers – Indigenous:
- Indigenous Wellness Clinic in Edmonton
- Dr James Makokis (South Common Medical Clinic in Edmonton)
*Please note, some clinics may not be accepting patients at this time. Contact the clinic directly to find out if they are accepting patients, have a waiting list, or can provide a referral.
Why am I included in the program?
In Alberta, individuals are included in population-based screening based on their age and the sex marker on their Alberta ID card.
| Cancer Screening Program | Biological sex marker on Alberta ID card | Age |
| Breast/chest cancer screening | Female | 45 to 74 |
| Cervical cancer screening | Female | 25 to 69 |
| Colorectal cancer screening | Female and Male | 50 to 74 |
How can I opt out of the Program?
There are two ways that individuals can opt out of the program:
1. Call Screening Programs at 1-866-727-3926. You will need to provide your personal health care number, name, and date of birth.
2. Change the sex marker on you Alberta ID card to match your gender identity and expression.
a. Information on how to do this can be found at https://www.alberta.ca/birth-record-sex-amendment.
b. For help with this process, you can make an appointment with one of the Trans ID Clinics listed below:
Calgary: Skipping Stone
Web: https://www.skippingstone.ca/id-clinics
Tel: (587) 333-4342
Email: info@skippingstone.ca
Edmonton: Student Legal Services of Edmonton
Web: https://www.slsedmonton.com/trans-id-project
Tel: (780) 492-8287
Email: slsoed@ualberta.ca
People of any gender identity or sexual orientation may need to get screened for cancer. It is recommended to speak with your healthcare provider about your personal cancer risk level and whether screening is right for you.
For More Information
Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Breast/Chest Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
Cervical Cancer Screening for the 2SLGBTQI+ Community
Download [info sheet] 
LGBTQ2S+/Sexual and Gender Diversity, Alberta Health Services
Sexual and Reproductive Health, Alberta Health Services
For 24/7 nurse advice or general health information, call Health Link at 811.
Breast Cancer Screening for First Nations People
The following resource about breast cancer screening was developed for First Nations people by the Alberta First Nations Information Governance Centre. Alberta FNIGC Breast Screening




